The Equitable Jab Blues – Word Jazz
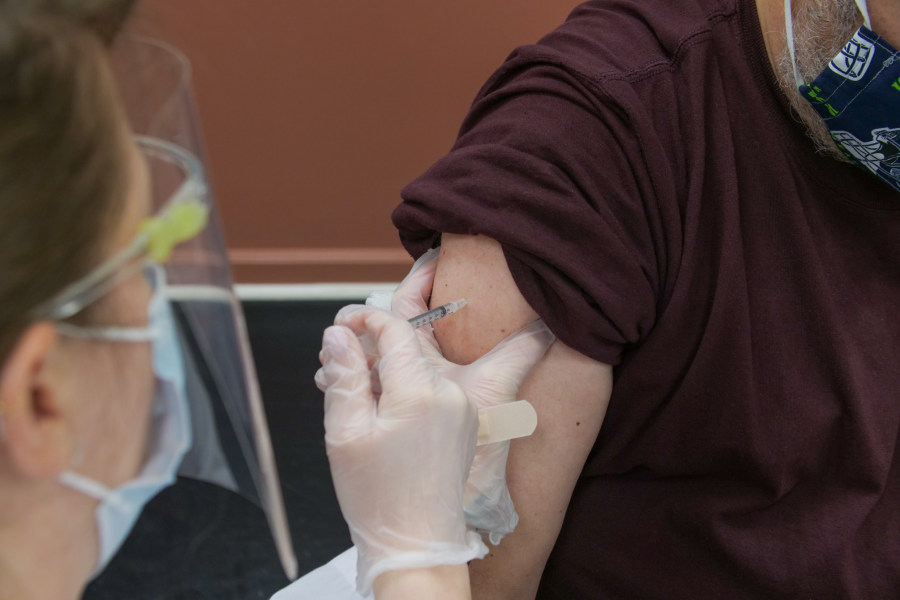


Going a bit nuts, a ray of hope, finding the vaccine, inequities galore. Get the…
Danny van LeeuwenJanuary 31, 2021







